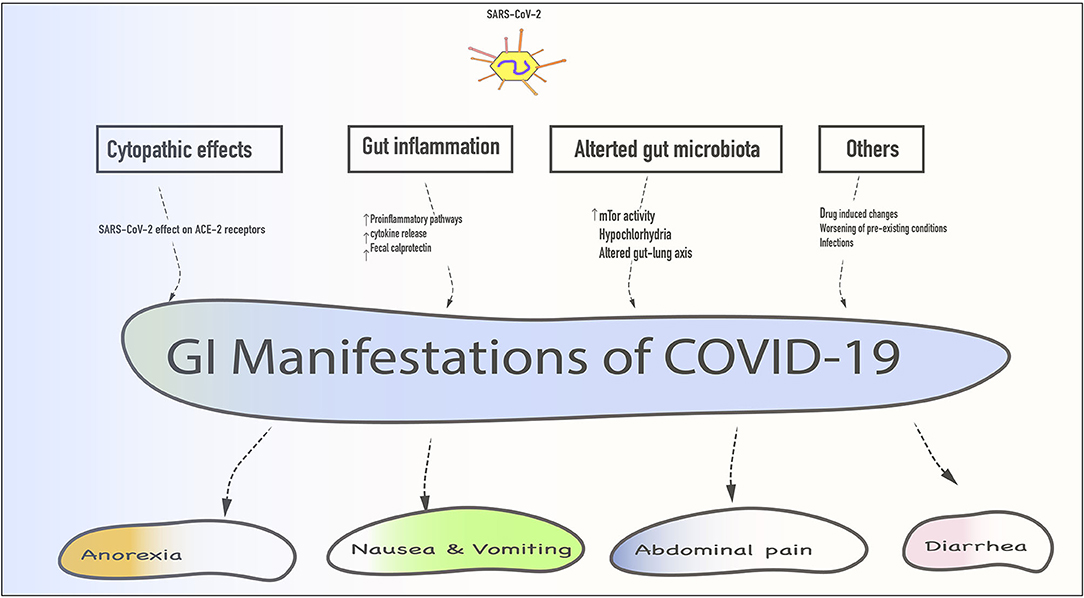
Some researchers suggest that gut dysfunction may exacerbate the severity of infection by enabling the virus to access the surface of the digestive tract and internal organs. These organs are vulnerable to infection because they have widespread ACE2—a protein target of SARS-CoV-2 for its possible routes of entry —on the surface. ACE2 is abundantly present in the epithelia of the lung and small intestine.
Several studies have already demonstrated that, when compared with healthy individuals, COVID-19 patients present a significantly reduced bacterial diversity and higher abundancy of opportunistic Streptococcus, Rothia, Veilonella, and Actinomyces compared to depleted levels of beneficial Agathobacter, Fusicatenibacter, Roseburia, and Ruminococcaceae UCG-013. Rothia was preeviously thought to contribute to the pathogenesis of pneumonia. Critically ill patients on mechanical ventilation who were given probiotics experienced decrease in viral colonization when compared with placebo. However, the efficacy of probiotics use in COVID-19 patients and other bowel remedies remains to be proved.
La Marca A, Capuzzo M, Paglia T, Roli L, Trenti T, Nelson SM. Testing for SARS-CoV-2 (COVID-19): a systematic review and clinical guide to molecular and serological in-vitro diagnostic assays. Reproductive biomedicine online. 2020 Jun 14.
Oshima T, Siah KT, Yoshimoto T, Miura K, Tomita T, Fukui H, Miwa H. Impacts of the COVID‐19 pandemic on functional dyspepsia and irritable bowel syndrome: A population‐based survey. Journal of gastroenterology and hepatology. 2020 Nov 16.
Sudre CH, Lee KA, Lochlainn MN, Varsavsky T, Murray B, Graham MS, Menni C, Modat M, Bowyer RC, Nguyen LH, Drew DA. Symptom clusters in Covid19: A potential clinical prediction tool from the COVID Symptom study app. MedRxiv. 2020 Jan 1.
Riphagen S, Gomez X, Gonzalez-Martinez C, et al. Hyperinflammatory shock in children during COVID-19 pandemic. Lancet. 2020;395:1607–1608.
Giacomet V, Barcellini L, Stracuzzi M, Longoni E, Folgori L, Leone A, Zuccotti GV. Gastrointestinal Symptoms in Severe COVID-19 Children. The Pediatric infectious disease journal. 2020 Aug 10;39(10):e317-20.
Cholankeril G, Podboy A, Aivaliotis VI, Tarlow B, Pham EA, Spencer SP, Kim D, Hsing A, Ahmed A. High Prevalence of Concurrent Gastrointestinal Manifestations in Patients With Severe Acute Respiratory Syndrome Coronavirus 2: Early Experience From California. Gastroenterology. 2020 Aug 1;159(2):775-7.
Gu, S.; Chen, Y.; Wu, Z.; Chen, Y.; Gao, H.; Lv, L.; Guo, F.; Zhang, X.; Luo, R.; Huang, C.; et al. Alterations of the Gut Microbiota in Patients with COVID-19 or H1N1 Influenza. Clin. Infect. Dis. 2020, 71, 2669–2678.
Dhar, D.; Mohanty, A. Gut microbiota and Covid-19- possible link and implications. Virus Res. 2020, 285, 198018.
Sudre CH, Lee KA, Lochlainn MN, Varsavsky T, Murray B, Graham MS, Menni C, Modat M, Bowyer RC, Nguyen LH, Drew DA. Symptom clusters in Covid19: A potential clinical prediction tool from the COVID Symptom study app. MedRxiv. 2020, June 16.
Kim HS. Do an Altered Gut Microbiota and an Associated Leaky Gut Affect COVID-19 Severity?. mBio. 2021 Feb 23;12(1).
Ferreira, C.; Viana, S.D.; Reis, F. Is Gut Microbiota Dysbiosis a Predictor of Increased Susceptibility to Poor Outcome of COVID-19 Patients? An Update. Microorganisms 2021, 9, 53.